What with my heart surgery scheduled for next Thursday, today I went in to the hospital for some “pre-admission” procedures and consultations in anticipation of that upcoming operation. The more minor of the procedures that I experienced today included a chest X-ray; an EKG (electrocardiogram); and bloodwork. Although I normally hate having blood taken, and although my heart sank when I saw how many vials the nurse was going to fill (which would mean that the needle would be in for a relatively long time), this morning’s bloodwork barely hurt at all. So that was an unexpected bonus.
My consultation regarding the anesthesia
It probably helped that I was distracted while the blood was being extracted from my vein; because while that was going on, a nurse was simultaneously briefing me on some details regarding the anesthesia that I’ll be given at the outset of my surgery. That hospital is nothing if not efficient. 🙂 Anyway, I did have a lot of questions for the nurse, in light of the fact that I’ve never been under general anesthesia before. She also gave me some instructions to help prepare my body for the anesthesia. (In addition to the standard requirement of fasting from midnight the night before the surgery, an example of those instructions was that from now until after the surgery, I shouldn’t taken any anti-inflammatory pain medications, commonly referred to as NSAIDs, which is an abbreviation for non-steroidal anti-inflammatory drug. In the United States, among the popular painkillers that are classified as NSAIDs are Advil and Motrin.)
Also during my colloquy with the nurse, I mentioned that I’m a singer and that I therefore hoped the anesthesiologists would go easy with the breathing tube that will be jammed down my throat during the surgery, in order to avoid damaging my vocal cords. (Yes, I told the nurse about my World Karaoke Tour. :)) Relatedly, we discussed how, as is standard in heart surgery, I’ll still be “intubated” (that is, the breathing tube will still be inserted down my throat) when I wake up in the operating room. While my surgeon believes in “extubating” (removing the tube) very quickly after the patient regains consciousness, I expressed concern that until the extubation occurs, I may feel like I’m choking. The nurse offered that if I want to minimize the risk of harm to my vocal cords, I should refrain from struggling with the breathing tube before it’s removed. Sound advice, I’m sure; but how will I have the presence of mind to remember it when I’ve just been knocked out for four hours and I’m feeling groggy and disoriented?
My CT-scan and a missed photographic opportunity
After all of that was finished, I had to walk several blocks to another of the hospital’s buildings, where I underwent a computed tomography scan, usually abbreviated as a CT-scan. My CT-scan involved the following steps:
• I drank several cups of water.
• An intravenous (IV) tube was attached to one of my veins.
• While lying on my back, I was slid into a cool machine with the appearance of a vertical donut. Via some blasts of radiation, images were taken of my chest, abdomen, and pelvis areas.
• A “contrast dye” was then injected into me through the intravenous tube, and more images were taken inside the donut-esque machine. You may have heard that when such a dye is pumped into a patient’s vein, the patient experiences a warm, tingly feeling throughout his body for a couple of minutes. That proved to be the case with me.
Things didn’t go completely smoothly during my CT-scan. When the radiologist initially jabbed the needle into my vein to create a pathway for attaching the IV tube — which was quite painful, by the way, as the needle was large — the vein “popped” (in the words of the radiologist), rendering it unsuitable for an IV connection. According to the radiologist, that’s not an unheard-of occurrence. So she had to remove the needle and call in another radiologist to find a suitable vein in my other arm. And I had to again endure the hurtful penetration of the needle. Admittedly, once the IV tube had been attached, the pain subsided.
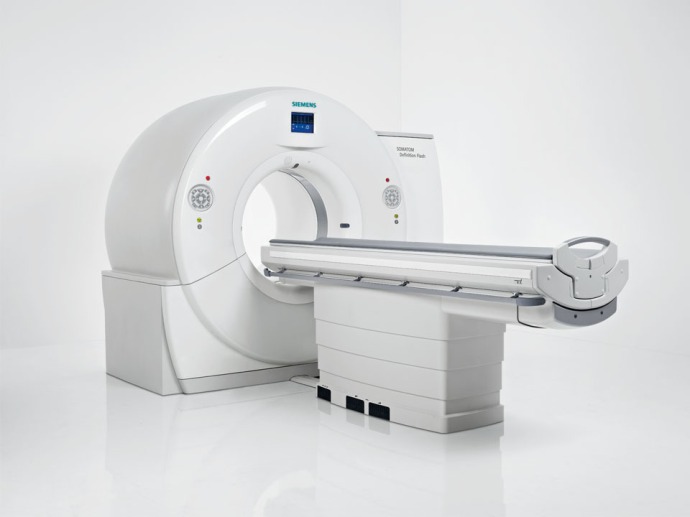
By the way, I would love to be able to show you a photo of the actual CT-scan machine that was used for my procedure. But I screwed up. I made a rookie mistake: upon entering the room where I was CT-scanned, I asked the radiologist if it would be okay to snap a quick pic of the machine that I would soon be slid into. She denied me permission, claiming that the hospital’s licensing agreement with Siemens, the manufacturer of the machine, precluded any photographing of Siemens’s equipment. I pointed out, to no avail, that Siemens would receive free publicity if I posted a photo of its product on my blog. 🙂 But really, my travels should have taught me that when you want to take a “forbidden” photo, you never give an authority figure the chance to say no. You just quickly and furtively aim your phone and release the shutter. I was even holding my phone in my hand as I walked into the room, but I stupidly thought that if asked the radiologist nicely, she would agree to let me take the requested photo. What made her denial especially disappointing was that, immediately above the donut-shaped portion of the machine was a video monitor that was displaying my name in large capital letters. (In case you’re wondering, the moniker that appeared was my actual name — it didn’t say “H-Bomb”). 🙂 It would have been so awesome to get a photo of the high-tech imaging machine with my name appearing on its screen; but sadly, that photo eluded me.
Here’s a photo that I found on the internet of a similar CT-scan device from the same manufacturer. The video screen is a little different, and more importantly it isn’t showing my name; but this photo is the best I could do for this blog post. 🙂
Next steps: catheterization, surgery, and recovery
One more pre-op procedure: the heart catheterization
On Wednesday, September 9, I’ll be returning to the hospital for a diagnostic procedure called a heart catheterization. In a “heart cath,” a tube with a tiny camera attached is inserted into an artery (in the case of my hospital, the femoral artery in the arm) and run all the way through the artery to my heart. The purpose of this test is to check for blockages. (I’ve been told that in view of my age, it’s unlikely that any blockages will be found; but in the event that any are identified, a device called a stent will be implanted in me several weeks after my main surgery.)
Although I’ve previously mentioned that I opted not to undergo the catheterization, my surgeon talked me into doing it when I met with him a couple of weeks ago. He explained that my only alternative would be a second CT-scan (separate from the one that I had today); and given the high dose of radiation that a single CT-scan entails, I didn’t want to be blasted with such radiation on multiple occasions. My surgeon added that the catheterization would be relatively quick, taking only about 15 minutes; that it would provide him with a superior quality image as compared to the hypothetical second CT-scan; and that 99% of his patients choose it.
My surgery and hospitalization
Immediately following the catheterization, I’ll be checked in to the hospital. Sometime later that day, I’ll be given consent forms to sign that set forth the risks of my surgery. I’m going to sign those forms without reading them, since it would probably be scary and upsetting to see all the risks spelled out in print. 🙂
Very early on Thursday morning, September 10 I’ll be awakened. At about 6:30 a.m., my parents and my good friend Heather will join me in the waiting area. An hour or so later, the anesthesia will be pumped into my body and I’ll be operated on. (If you’re new to this saga, the type of surgery that I’m having is a mitral valve repair; for background on why I need the surgery, go here.) Roughly four hours after that, I’ll wake up in the O.R. and will be extubated (hopefully very quickly). 🙂
Then I’ll be taken to the recovery room, an intensive care-type setup containing a number of other patients, in which I’ll spend the night. While I’m in the recovery room, numerous tubes that were hooked up to me while I was anesthetized will remain connected to me. Those tubes will include between one and three tubes running into my chest, to drain fluid; a tube connected to my neck; a urinary catheter; and of course the standard IV tube. Nurses will constantly be swinging by to check my vital signs. The recovery room will be busy and loud.
On Friday morning, September 11, assuming that there’ve been no complications, I’ll be moved to a regular hospital room (on what the cardiology department refers to as “the floor”), and all of the tubes except the IV will be removed. Things will become much more comfortable and serene at that point. Moreover, once I’ve been relocated to the floor, the staff will have me taking walks around the corridors as quickly as possible. It’s also expected that because I’m having the less-invasive, robotically-assisted version of the valvular repair surgery, my need for hardcore pain meds in the days immediately following the operation will be relatively low. Of course, as I’ve heard many times from many medical professionals over the past few months, every patient is different.
My home recovery, and beyond
If all goes well, I’ll be discharged from the hospital on Sunday morning, September 13. (The surgeon said it’s possible I could be held over until Monday the 14th, but that a Sunday release is more likely.) It’s expected that I’ll be able to return to work between two and three works after my discharge.
In the interim, I won’t just be lying in bed; I’ll be under doctor’s orders to take two walks per day to Central Park, and to gradually increase the length of those walks. Aside from the general importance of exercise, these strolls will be an important part of rebuilding the stamina of my cardiovascular system. (However, I’ll be required to wait several weeks before resuming working out on the eliptical machine at my local gym.) In addition to the walks, at least during the first week or two, I’ll receive a small number of home visits from a nurse to check up on me; and also for a week or two, every day during my waking hours, I’ll be required to breathe into a device called a spirometer on an hourly basis. (The purpose of those breathing exercises is to help clear mucus from my lungs.)
I’ll also be on some medications for a while after the surgery. For one month, I’ll be taking a blood-thinner (described by my surgeon as a “super aspirin”); and for three months, I’ll be taking regular aspirin and beta blockers.
Within four weeks after my discharge, I should be sufficiently recovered to receive medical clearance to travel. I’m hoping to attend my 20-year law school reunion at Georgetown University Law Center the weekend of October 16-18 (in fact, I’ve already bought my ticket for that); my surgeon is confident that I’ll be able to make it to the reunion. And as the surgery recedes further into my rear-view mirror, I’ll be able to resume my World Karaoke Tour; my future trips that are in various stages of planning include visits to Rome, Italy in late November; Charleston, South Carolina for several days surrounding New Year’s 2016; Nassau, Bahamas in mid-February; and the trifecta of China, Taiwan, and North Korea in late May to early June.
During my hospitalization and recovery, I’ll post updates when warranted. (I’m also still not sure whether I’ll be bringing my laptop to the hospital, so I may not be able to blog from there at all.) I appreciate your company as you join me for my medical adventure.



I’m about to read your article but I had to comment how stylish you look in that pinstriped hospital gown.
LikeLike
Yes, a CT scanner with your name on it *would* have been cool 😜. How’s life in the cath lab? I’m proud of you. Take more pics. I wish we were there!!! I am confident you will be up and ambulating in the hallways in no time. Go team MVP!
LikeLike
So, it’s been several weeks now. How are you feeling? We haven’t read anything since this article.
LikeLiked by 1 person
@David C.: It’s been a slow recovery with ups and downs, although the general trend has been upward. I’ll probably have a post up in early November about the whole operation and recovery process.
LikeLike
Glad to hear it. Get well soon.
LikeLike